Have you been feeling mild stomach pain, changes in bowel habits, or unusual bloating, and wondering if it could be something more serious?
Many people ignore early symptoms of diverticulosis because they seem minor at first. But recognizing the symptoms of diverticulosis early can prevent complications and protect your digestive health. Diverticulosis is common among adults over 40 in the United States, yet most people do not know they have it until they experience discomfort.
In this guide, we will explain the early symptoms, what causes them, how doctors evaluate the condition, and when to see a gastroenterologist.
Understanding the causes of diverticulosis, available treatments, and warning signs can help you take action before problems become serious.
Table of Contents
What Is Diverticulosis and Why Does It Develop?
Diverticulosis happens when small pouches called diverticula form in the wall of the colon. These pouches develop due to pressure inside the intestine, often linked to diet and aging. While many people have no symptoms, early signs of diverticulosis can appear gradually.
How Common Is Diverticulosis in the United States?
According to the National Institute of Diabetes and Digestive and Kidney Diseases, more than 30% of U.S. adults between the ages of 50 and 59 and more than 70% of those older than age 80 have diverticulosis. Many do not experience symptoms of diverticulosis until inflammation or irritation occurs.
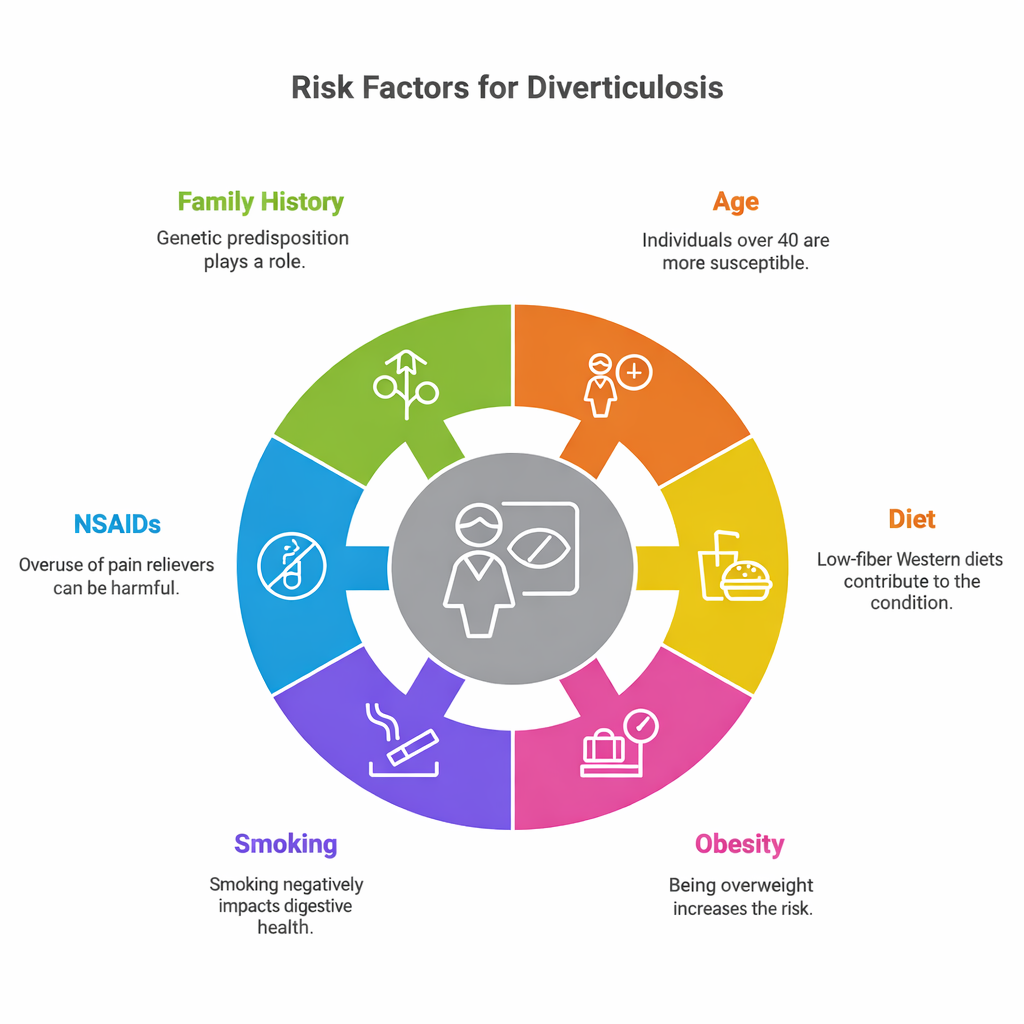
The Main Diverticulosis Causes
Several causes of diverticulosis increase risk:
- Low-fiber diet
- Chronic constipation
- Aging colon wall
- Obesity
- Sedentary lifestyle
A low-fiber diet increases pressure inside the colon. Over time, this pressure pushes weak spots outward, forming diverticula.
What Are the Symptoms of Diverticulosis?
Early symptoms are often mild and easy to ignore. But recognizing the symptoms of diverticulosis early can prevent complications such as diverticulitis.
The most common diverticulosis symptoms include mild abdominal discomfort, bloating, constipation, and irregular bowel movements.
- Mild Lower Left Abdominal Pain – Pain is often dull and located on the lower left side of the abdomen. It may come and go, and it may worsen after meals.
- Changes in Bowel Habits – Constipation is common. Some patients alternate between constipation and diarrhea. These shifting bowel patterns are often early symptoms.
- Bloating and Gas – Gas buildup and abdominal fullness can occur due to slowed movement in the colon.
Tip: If discomfort improves after a bowel movement, it may indicate pressure-related diverticulosis symptoms.
Early Warning Signs That Should Not Be Ignored
Some symptoms of diverticulosis are mild, but certain signs require medical attention.
Persistent abdominal pain, fever, nausea, or rectal bleeding may signal inflammation or infection.
When Diverticulosis Becomes Diverticulitis
Diverticulitis occurs when pouches become inflamed or infected. Symptoms become sharper and more intense.
According to NIDDK.gov, about 5% of people with diverticulosis develop diverticulitis.
Signs That Require Immediate Evaluation
- Fever above 100.4°F
- Severe abdominal pain
- Vomiting
- Blood in stool
If you experience these symptoms, do not delay care.
How Diverticulosis Is Different From Diverticulitis
Diverticulosis and diverticulitis are related but not the same condition. Diverticulosis refers to the presence of small pouches in the colon, while diverticulitis occurs when those pouches become inflamed or infected. Understanding the difference helps patients recognize when mild symptoms may be turning into a medical emergency.
What Is Diverticulosis?
Diverticulosis is a structural condition. It means small balloon-like pouches have formed in weak areas of the colon wall. Many people with diverticulosis do not feel anything at all.
The causes of diverticulosis are mainly linked to long-term pressure within the colon. A low-fiber diet, chronic constipation, aging, and physical inactivity increase the risk. In most cases, treatment for diverticulosis focuses on lifestyle changes rather than medication or surgery.
What Is Diverticulitis?
Diverticulitis is a complication of diverticulosis. It happens when one or more pouches become inflamed or infected.
This is when symptoms of diverticulosis progress from mild discomfort to sharp, severe pain.
Common signs of diverticulitis include:
- Sudden and intense lower left abdominal pain
- Fever
- Nausea or vomiting
- Tender abdomen
- Elevated white blood cell count
Diverticulitis often requires antibiotics and sometimes hospitalization. Advanced treatments may be needed if complications develop.
Key Clinical Differences Patients Should Know
Understanding the medical difference can help you know when to seek care.
Diverticulosis:
- Structural condition
- Often, there is no severe pain
- No infection present
- Managed with fiber and monitoring
Diverticulitis:
- Active inflammation or infection
- Sharp pain and fever
- May require antibiotics
- Risk of complications like abscess or perforation
One of the most important points is this: mild diverticulosis symptoms should not cause fever. If fever appears, it may indicate diverticulitis.
Why This Difference Matters for Your Health
Many patients delay care because they believe all digestive pain is the same. But early symptoms are very different from those of infected diverticulitis.
If you understand the causes and monitor your symptoms carefully, you can reduce the risk of complications.
Early diagnosis allows doctors to recommend preventive treatments before inflammation develops.
Ignoring warning signs increases the risk of:
- Abscess formation
- Intestinal blockage
- Colon perforation
- Emergency surgery
That is why knowing the difference is not just a matter of medical knowledge; it can protect your life.
How Gastroenterologists Diagnose Diverticulosis
Diagnosis often occurs during routine colonoscopy screening. Many cases are found before symptoms appear.
Doctors evaluate diverticulosis symptoms using imaging tests.
Colonoscopy
A colonoscopy allows direct visualization of diverticula in the colon.
CT Scan
CT imaging helps detect inflammation and rule out complications.
Medical History and Physical Exam
Your doctor will ask about symptoms, bowel changes, diet, and family history.
How to Relieve Symptoms of Diverticulosis?
Mild diverticulosis symptoms can often be managed with lifestyle adjustments. Increasing fiber intake and hydration reduces pressure inside the colon.
Dietary Changes
The American Gastroenterological Association (AGA.org) recommends 25–30 grams of fiber daily.
Fiber sources:
- Whole grains
- Vegetables
- Beans
- Fruits
Hydration
Water helps fiber move smoothly through the colon.
Exercise
Regular movement improves bowel regularity.
Medical Diverticulosis Treatments
For recurring discomfort, doctors may recommend:
- Fiber supplements
- Stool softeners
- Antispasmodic medications
Advanced treatments are needed only if complications develop.
Practical Insight: Do not suddenly increase fiber. Gradually raise intake to avoid worsening diverticulosis symptoms.
When to See a Gastroenterologist?
If symptoms of diverticulosis last more than a few days or keep returning, evaluation is important.
Persistent diverticulosis symptoms should not be ignored, especially in adults over 40.
High-Risk Individuals
You should consult a specialist if you:
- Have a family history of colon disease
- Experience rectal bleeding
- Have unexplained weight loss
- Have ongoing abdominal pain
Early evaluation allows proper treatments before complications occur.
Key Takeaways
- Diverticulosis is common in adults over 50 in the U.S.
- Early diverticulosis symptoms include bloating, constipation, and mild pain.
- Persistent symptoms of diverticulosis require medical evaluation.
- Causes of diverticulosis include a low-fiber diet and aging.
- Proper treatments focus on fiber, hydration, and monitoring.
- Severe pain or fever may signal diverticulitis.
Conclusion
Digestive discomfort should never be ignored, especially when it may involve early symptoms. Recognizing diverticulosis symptoms early allows proper diagnosis and timely diverticulosis treatment.
At Gastroenterology Associates, our board-certified gastroenterology specialists provide advanced digestive care tailored to each patient. With modern diagnostic tools and patient-centered treatment plans, we focus on preventing complications and improving long-term gut health.
If you are experiencing ongoing symptoms of diverticulosis or are unsure about your digestive health, seeking a professional evaluation can help protect your colon and prevent serious complications.
Why wait until mild discomfort turns into a medical emergency?
FAQs
Can diverticulosis cause bleeding, and what should I do if I notice blood in my stool?
Yes, diverticulosis can sometimes cause rectal bleeding if a small blood vessel in a diverticulum ruptures. This bleeding is usually painless but may appear as bright red or maroon blood in the stool. If you notice blood in your stool, seek prompt medical attention to rule out serious complications and receive appropriate care.
Is it possible to have diverticulosis without any symptoms?
Absolutely. Most people with diverticulosis do not experience any symptoms and may only discover the condition during routine screenings, such as a colonoscopy. However, even if you have no symptoms, maintaining a healthy lifestyle can help prevent complications.
How is diverticulosis different from irritable bowel syndrome (IBS)?
While both diverticulosis and IBS can cause abdominal discomfort and changes in bowel habits, they are different conditions. Diverticulosis involves the formation of pouches in the colon wall, whereas IBS is a functional disorder affecting how the colon moves. A gastroenterologist can help determine the cause of your symptoms through evaluation and testing.
Can certain medications make diverticulosis symptoms worse?
Yes, some medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs) and steroids, may increase the risk of diverticulosis complications or worsen symptoms. Always consult your doctor before starting or stopping any medications if you have diverticulosis.
What lifestyle changes can help prevent diverticulosis from progressing or causing symptoms?
To help prevent diverticulosis from worsening, adopt a high-fiber diet, stay well hydrated, exercise regularly, avoid smoking, and maintain a healthy weight. These lifestyle choices support colon health and may reduce your risk of developing complications.
Can stress or anxiety make diverticulosis symptoms worse?
Stress and anxiety do not directly cause diverticulosis, but they can worsen gastrointestinal symptoms like abdominal discomfort, bloating, and changes in bowel habits. Managing stress through relaxation techniques, exercise, and healthy sleep habits may help reduce symptom flare-ups.
Are there specific foods I should avoid if I have diverticulosis?
There is no universal list of foods to avoid, but some people find that certain foods can trigger their symptoms. It is generally recommended to eat a high-fiber diet, but if you notice discomfort after consuming foods like seeds, nuts, or popcorn, discuss your diet with your doctor or a registered dietitian. Personalized guidance can help you manage symptoms while maintaining good nutrition.
Are You Ready to Act on Early Diverticulosis Symptoms?
If you are experiencing early symptoms of diverticulosis or ongoing symptoms, do not ignore them.
Schedule an evaluation with a trusted gastroenterologist today. Visit us and request an appointment. Early diagnosis and personalized treatment for diverticulosis can protect your long-term digestive health.
Your gut health matters. Are you ready to take control of it today?