
Many Americans schedule appointments but leave without clear answers. They nod politely. They accept routine advice. But when it comes to something as serious as colon cancer, asking the right questions can change outcomes.
According to the Centers for Disease Control and Prevention, colorectal cancer is the second leading cause of cancer death among cancers that affect both men and women in the United States. The American Cancer Society estimates over 150,000 new cases annually.
This is not rare. This is not distant.
The most powerful thing you can do is ask better questions.
Table of Contents
Why Is Colon Cancer Screening Right for Me?
Every patient has a different risk level based on age, family history, and health conditions. Colon Cancer Screening decisions should be personalized. Asking direct questions ensures your plan matches your risk.
Do not assume you are “average risk.” Ask your gastroenterologist:
- Am I considered average or high risk?
- What factors increase my personal risk?
- Does my lifestyle affect my screening schedule?
- Should I consider genetic testing?
Many patients do not realize that conditions like inflammatory bowel disease or a family history of polyps change recommendations.
This conversation is the foundation of prevention.
Quick Fact: The U.S. Preventive Services Task Force recommends routine screening starting at age 45 for most adults.
What Is the Right Colon Cancer Screening Age for Me?
The age for colon cancer screening is not the same for everyone. Family history and medical background can shift timelines. Clarifying your starting age reduces missed early disease.
The standard starting point is 45. But you should ask:
- Should I start earlier due to family history?
- If a relative was diagnosed young, how does that affect me?
- How often should I repeat testing?
If any of your parents were diagnosed at 50, your timeline may begin earlier.
Do not rely on general guidelines. Make it personal.
Which Screening for Colon Cancer Test Is Best for Me?
There are multiple screening options available. Screening for colon cancer can include stool tests or a colonoscopy. Understanding differences helps you choose wisely.
Ask clearly:
- What test do you recommend and why?
- What is the accuracy rate?
- What are the risks?
- What preparation is required?
Colonoscopy
- Examines the entire colon
- Removes polyps immediately
- Usually repeated every 10 years if normal
Stool-Based Tests
- Non-invasive
- Must be done more frequently
- Positive results require a colonoscopy
According to many studies, removing precancerous polyps during colonoscopy prevents cancer from forming.
That makes your test choice strategic rather than routine.
Pro Tip: Ask your doctor about their adenoma detection rate. Higher rates mean better detection of precancerous polyps.
What Signs of Colon Cancer Should I Watch For Between Visits?
Symptoms may not appear early. Recognizing signs of colon cancer allows faster intervention. Reporting changes early improves outcomes.
Ask:
- Which symptoms require urgent evaluation?
- How long should bowel changes last before concern?
- Is occasional bleeding always serious?
Common warning signs include:
- Blood in stool
- Persistent abdominal discomfort
- Unexplained weight loss
- Fatigue
- Change in bowel habits lasting weeks
Many colon cancer symptoms overlap with less serious issues. That is why evaluation matters.
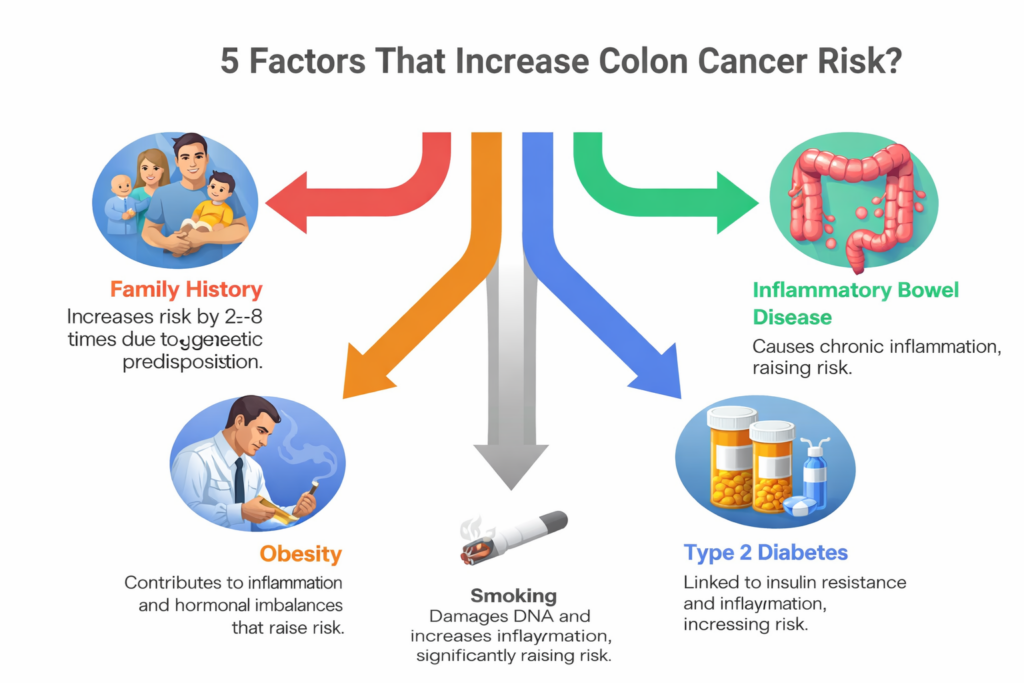
Understanding Your Personal Risk Factors for Colon Cancer
Risk is shaped by age, ethnicity, genetics, medical history, and lifestyle. Discussing these factors allows targeted prevention.
Important factors to review:
- Family history of colon or rectal cancer
- History of polyps
- Inflammatory bowel disease
- Type 2 diabetes
- Obesity
- Smoking
- High red meat intake
African Americans have higher incidence and mortality rates compared to other groups.
Ask your doctor:
- Does my ethnicity increase my risk?
- Does my past medical history change my screening frequency?
- Should I consider earlier surveillance?
How Does My Lifestyle Affect My Risk?
Diet, weight, and lifestyle habits influence the development of colon cancer.
Ask directly:
- Does my diet increase risk?
- Should I reduce processed meats?
- How much exercise lowers risk?
- Does alcohol consumption matter?
Research from the National Cancer Institute links obesity, physical inactivity, and high red meat consumption to increased risk.
Lifestyle does not replace testing. It supports it.
If Cancer Is Found, What Happens Next?
Treatment depends on the stage and tumor location.
Ask:
- What stage would require surgery only?
- When is chemotherapy necessary?
- What are the survival rates by stage?
- How soon would treatment begin?
The earlier cancer is detected, the simpler the treatment plan.
Key Takeaways
- Colon cancer often develops without early symptoms.
- Asking detailed questions personalizes prevention.
- Screening timelines vary by risk.
- Lifestyle impacts colon health.
- Early detection dramatically improves survival.
- A normal test still requires follow-up planning.
Conclusion
You cannot prevent what you refuse to discuss.
Colon cancer is serious, but it is often preventable. The difference between early detection and late diagnosis can come down to one conversation and the questions you ask.
At Gastroenterology Associates, patient care focuses on prevention, early diagnosis, and personalized digestive health strategies.
The right time to act is before symptoms appear.
Frequently Asked Questions
1. What should I do if I have a family history of colon cancer?
If you have a family history of colon cancer, inform your gastroenterologist early. They may recommend earlier screening and genetic counseling.
2. Can I choose a non-invasive screening method instead of a colonoscopy?
Yes, stool-based tests such as FIT, FOBT, or Cologuard exist, but abnormal results require colonoscopy follow-up.
3. What are the possible risks of a colonoscopy?
Colonoscopy is generally safe. Minor bloating or bleeding may occur, and rare complications include colon perforation.
4. How can I reduce my risk of developing colon cancer?
Maintain a healthy weight, stay active, eat fiber-rich foods, limit processed meat, avoid smoking, and reduce alcohol.
5. What does it mean if my colonoscopy finds polyps?
Polyps are growths in the colon lining. Removing them during colonoscopy prevents many colon cancers.
Are You Asking the Right Questions About Your Colon Health?
If you are in the United States and want clarity about your risk, testing schedule, or symptoms, now is the time to act.
Contact us and schedule your consultation today.
Because if you are not asking these questions now, when will you?






